- Sponsored Content

Bunions (hallux valgus) are common and range from a mild, purely cosmetic issue to quite a debilitating, painful deformity. The word ‘bunion’ comes from the Greek, meaning turnip, and refers to the bump on the inside aspect of the big toe joint.
Who gets bunions?
Women are affected roughly fifteen times more than men and there is a hereditary element (you are more likely to be affected if your grandmother had bunions). The major factor however is poor footwear; pointy, high heeled shoes being the main culprit. This was demonstrated beautifully in a study from the 1950s: at that time roughly half of the population of Hong Kong wore shoes and half didn’t. Hallux valgus was seventy times more prevalent in the shoe-wearing population.
What non-surgical things can I do?
Most importantly, wear shoes that are wide enough for your feet. If you are unsure, you can trace the outline of your foot on a piece of paper (whilst standing) and then put your shoe over it. If the shoe is narrower than your foot, it is not good for daily use. High-heeled shoes cause you to load the front of your foot (which makes bunions worse) and tend to be very narrow in the ‘toe box’ so should only be for special occasions ideally.
Having a tight calf also causes forefoot overload so stretching can help. Splints, spacers and taping unfortunately cannot correct an existing deformity but may help to slow its progression. Custom-made orthotics from a reputable podiatrist can be useful.
When should I consider surgery?
You never have to have surgery as long as you can manage the symptoms with simple measures. Hallux valgus does tend to get worse over time, but it never gets so bad that it can’t be fixed (despite what some surgeons may tell you), so there is no hurry. The time to consider it is when your life/lifestyle is affected enough to undergo the associated hassles and minor risks.
What does surgery involve?
There are over 100 operations described but maybe six or seven, including some minimally invasive techniques, are in common usage today. Which procedure is recommended depends on several technical factors and is tailored to the individual. In general, surgery involves cutting and shifting the bone or fusing the joint (or both) to straighten the toe and improve the foot biomechanics. The success rate of modern procedures is high.
What’s the recovery?
Your grandma may have told you that her bunion surgery was excruciatingly painful but thankfully, with modern techniques, this is no longer true!
With most procedures, patients can walk straight away in a post op shoe (worn for six weeks). Swelling in the foot takes longer to settle than other parts of the body and may take a few months to fully resolve. Running is usually possible between three to six months depending on the procedure required and how keen you are to get back.
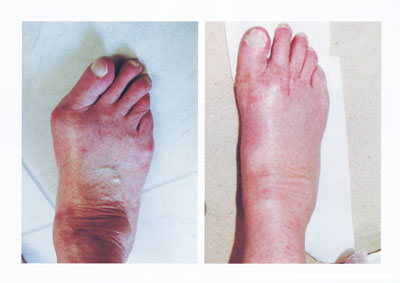
Before and six weeks after hallux valgus (and lesser toe) surgery. The foot is always still a bit swollen at this stage but note the alignment correction.

Dr Chris Pearce is an Orthopaedic Surgeon at Altius Clinic specialising in foot and ankle conditions. He is the author of several scientific studies, articles and book chapters on tendinopathies of the foot and ankle.
altiusclinic.sg

Altius Clinic Sports and Orthopaedic Surgeons
290 Orchard Road, #09-11/12 Paragon, 238859
contact@altiusclinic.sg
+65 8500 3961 +65 6970 1518








